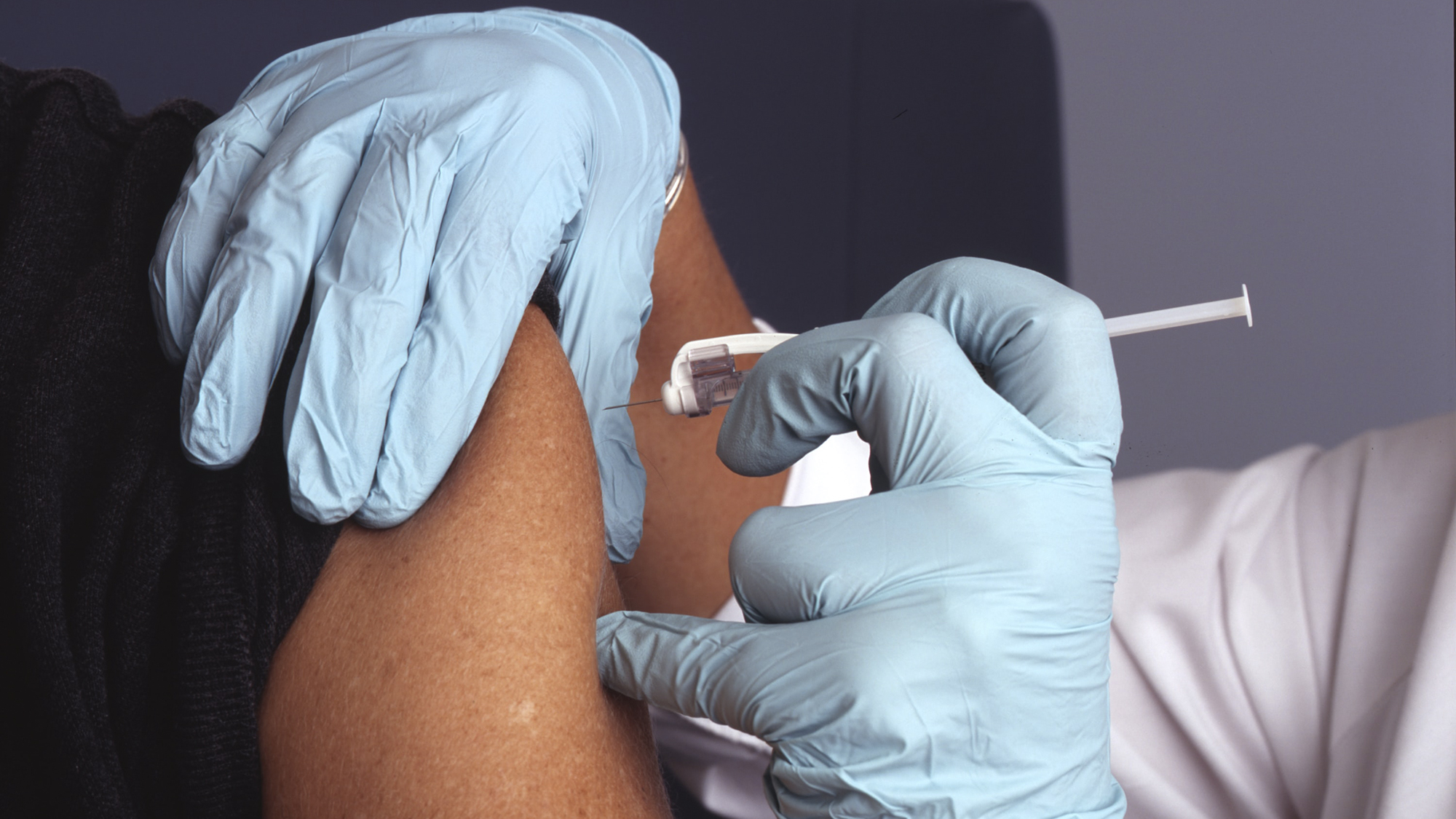
In Spain, we have entered the “new normality” after 99 days in a state of emergency. We have been stroked by a health crisis with precedents that, in our country, go back a century until the time of the Spanish Flu epidemic. In this new stage, the use of masks and physical safety distance will be measures that will be maintained until the COVID-19 vaccine arrives.
But once it is within our reach, and after the consequences experienced worldwide, will there be people who will not want to be vaccinated? And, if so, what are the reasons could drive them to take this decision?
Vaccines yes or no, a long-running debate
If we look at flu vaccine immunization coverage in Spain, only 55.7% of people at risk (over 65 years) were vaccinated in the 2017-2018 season, which is 10% less than 8 years before. In countries like the USA, this percentage is 59.6% in this same season. While we would expect these values to be similar to those for diphtheria, pertussis and tetanus vaccine, which accounted for about 97% in both countries in 2018, there is a tendency not to prioritize protection against this seasonal virus which causes between 290,000 and 650,000 deaths globally each year.
It is imperative to be clear about the importance and benefits of vaccination against diseases that still constitute a risk for the population.
But, what could be the reason behind vaccine’s rejection?
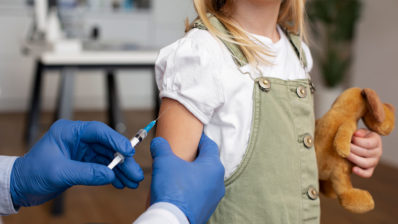
- A sense of false security about certain diseases that have been eradicated precisely thanks to vaccines, or that do not feel lethal to many of us, such as influenza. An example of this is diphtheria, a bacterial disease whose impact is minimal in countries of the global north. Since it is currently not a real threat to Western society, one might consider it pointless to get vaccinated. However, in 2015 an unvaccinated child died in Olot (Girona) from this disease. To avoid similar cases, it is imperative to be clear about the importance and benefits of vaccination against diseases that still constitute a risk for the population.
- Fear of adjuvants. These are substances added to vaccines in controlled amounts and harmless to humans, in order to increase immunogenicity. In many cases, misinformation and the perception that adjuvants are foreign elements, such as aluminium, feed the mistrust of the population and can lead to vaccination rejection, simply because they do not understand how they work. The same is true for many of the additives found in food products.
These arguments against vaccines are in general complemented by others that have emerged because of the pandemic we are experiencing and because of how this health crisis is being managed.
SARS-CoV-2 vaccine particularities
One day we are told that we have to disinfect all our groceries and the next day that we do not need to. We are seeing how more than 2000 scientific articles about this virus are published weekly, but not all its mechanisms of infectivity are yet known. We are witnessing how science is done, how a new pathogen is researched in real time. And that can be overwhelming, because scientific observations are not the ground truth, but rather the result of trial and error. We make many mistakes until we understand the nature of the problem we are facing, and from there, if it is a threat to us, we start looking for solutions. And precisely, seeking solutions to a virus that is already causing a global pandemic means working against the clock.
We are witnessing how a new pathogen is researched in real time. And that can be overwhelming, because scientific observations are not the ground truth, but rather the result of trial and error.
The magnitude and urgency of the problem has led to some peculiarities in the research for a SARS-CoV-2 vaccine, that could pose a threat to its acceptance:
- clinical trials’ adaptation. In order to have a solution as soon as possible, phases that are usually consecutive are now overlapping, or the vaccine is produced before it has been shown to be effective, as in the case of the vaccine developed by the University of Oxford. For example, the European Medicines Agency has already announced that SARS-CoV2 vaccines will go through a fast-track approval phase, potentially bypassing the standard approval process to allow their commercialisation under an emergency authorisation. Concerns about whether these changes will affect the safety of the vaccine may generate a sense of disapproval.
- the economic interest behind its production and the doubt about its availability worldwide. The discovery and development of new drugs and vaccines by the pharmaceutical industries is not only to serve scientific and/or medical interests, but also economic prosperity, as they are for-profit companies subject to the laws of the market. This is true even in emergency situations, such as the current COVID-19 pandemic, where countries around the world are facing the same problem and need their doses of the vaccine.
Facing the future
The end of the confrontation between the arguments against vaccines and the scientific community requires a bridge, a debate that generates its own informed, contrasted, and critical opinions. Only in this way can we collaborate in the construction of an empathetic and cooperative society. We believe that this communication must be transparent, making clear that there are economic benefits involved, but always safeguarding the effectiveness of the final product: the vaccine.
If, in spite of this, a part of society refused to vaccinate, would it be ethical to force people to get a shot?
About the authors:
This piece was written by Aritz Lafuente, Mireia Codina, Morena Pinheiro and Sergi Campos, students of the Master’s Degree in Multidisciplinary Research in Experimental Sciences at BIST-UPF. Each of them comes from a different scientific branch, but they are all united by science. On their Twitter account @VacciBate they talk about vaccines, trying to create an online debate about their benefits and their risks.



I have a very very ! Severe phobia and do not want any injections if there was an oral form of covid19 vacine I would say ok but no way am I having injections.
I feel the same way, to the point where I make the Dentist drill without injecting Lidocaine or Novocaine. That is how much I detest being impaled by needles. I refuse to believe there is not a way to get medications into your system without using needles.
Why would anyone trust the WHO or any Government? They have lied consistantly through the epedemic.The media surpress or promote there own agenders , so cannot be trusted. I would sooner take my own country to task then take a vaccine.
I don’t trust the rush put in finding the so called cure. I’d rather wait for the lab rats taking the cure. Side effects?
I don’t want to put something in my body that I don’t even know the side effects of it.
No injections for me.
Hw about Dr Bonne Henry and the others take it 1st…..
Im not sure about having this vaccine. It as been rushed and unroll I know for sure what side effects I don’t want it. I have copd and my breathing isn’t good atm.
Some people are citing Godly principles for not taking the vaccine. If people don’t want the vaccine this there business but I find something wrong with people using God not to take the vaccine. I will have faith in the system and take the vaccine once FDA approves it. Thank you
In my opinion NO One has the right to force a jab on anyone.A persons body is their own business if they don’t want a vaccine so be it ,if they catch covid it’s their business right!The issue here is choice and not taking any persons right to choose way.we have a vaccine if people choose not to have it that’s their right.
I don’t understand why it is been offered as after having it still need to social distance still wear mask and you can still get COVID. It is not a cure and how have they found it so quick when they so-called didn’t know how it started.